- 2026
CPR VAM • All Rights Reserved.

The American Heart Association (AHA) Pediatric Advanced Life Support (PALS) Algorithm provides a structured, evidence-based approach for managing pediatric emergencies. It guides clinicians in the rapid assessment and treatment of life-threatening conditions such as respiratory failure, shock, arrhythmias, and cardiac arrest in infants and children.
The 2025 AHA updates emphasize early recognition of deterioration, high-quality CPR with minimal interruptions, and improved airway and ventilation strategies. The algorithm follows a systematic cycle of evaluate, identify, intervene, and reassess, ensuring coordinated team response, reduced errors, and improved outcomes in high-acuity pediatric resuscitation settings.

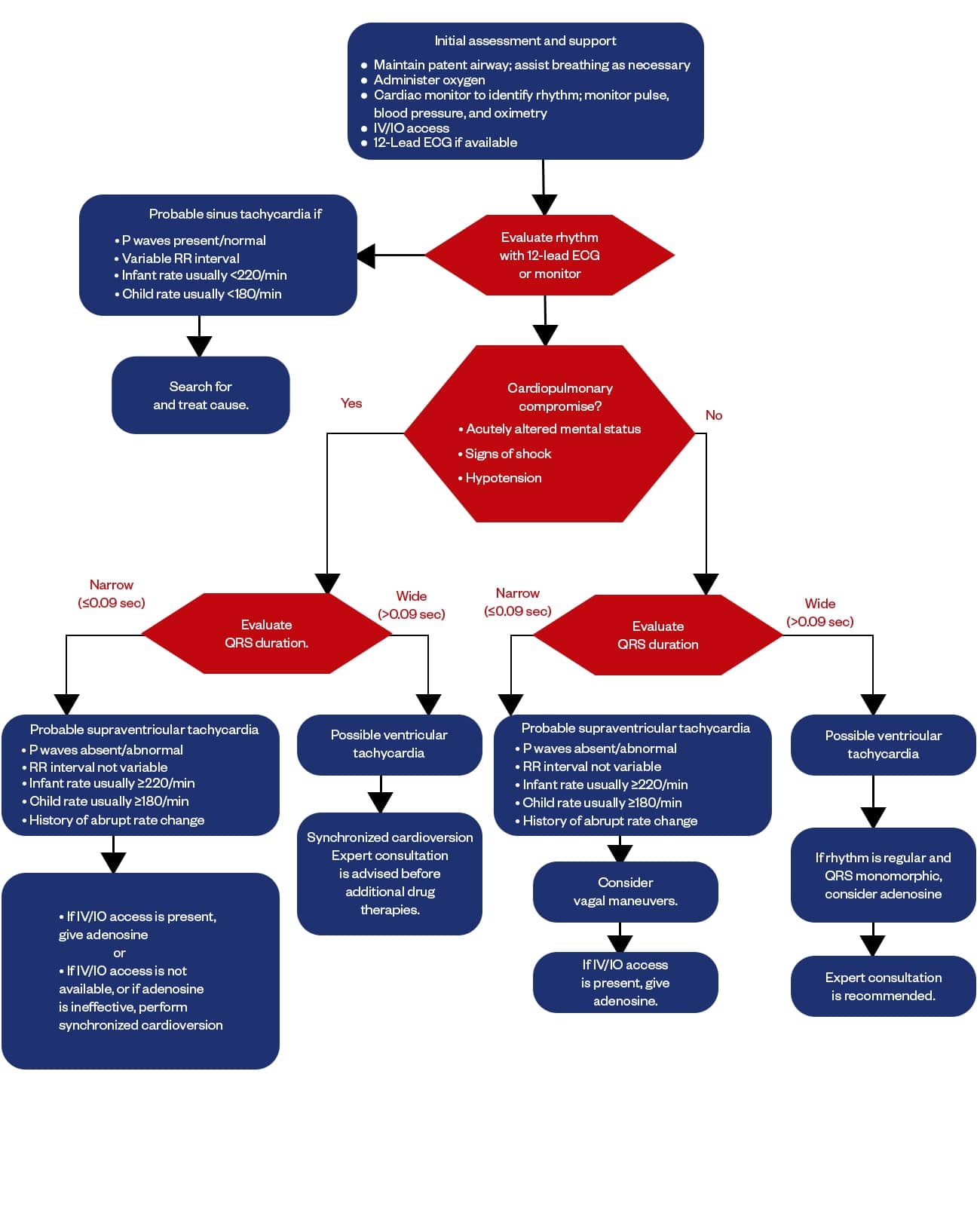
Pediatric tachycardia refers to the condition of a faster heartbeat rate, exceeding the upper limit of the normal rate for a child’s specific age group. This makes it essential to know the normal heart rate for children at first to determine if the child is tachycardic or not.
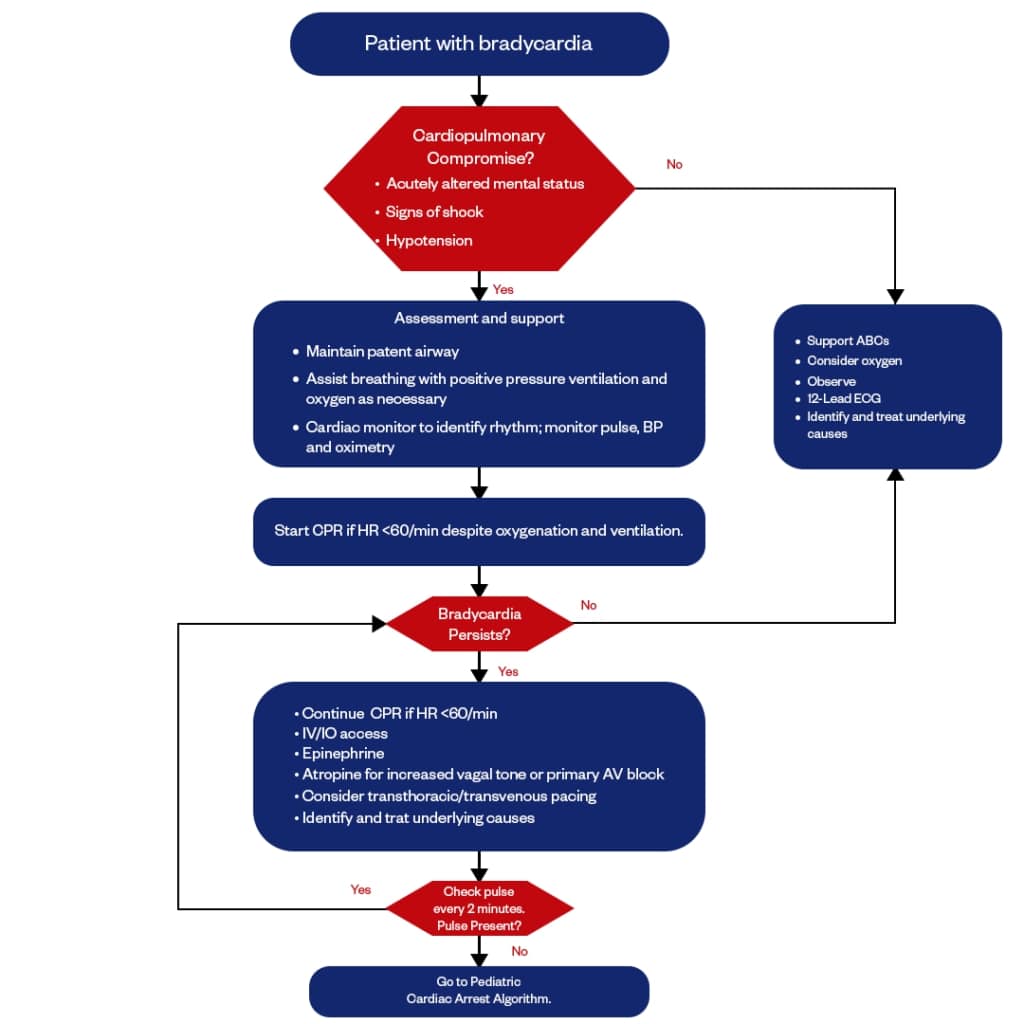
Pediatric bradycardia refers to a heart rate that is slower than the normal range for a child’s age, differing among infants, younger children, to adolescents. It results from several causes that may be heart-related or other underlying issues, such as low oxygen level (hypoxia), hypothermia, hypotension, or electrolyte imbalance.

Pediatric bradycardia refers to a heart rate that is slower than the normal range for a child’s age, differing among infants, younger children, to adolescents. It results from several causes that may be heart-related or other underlying issues, such as low oxygen level (hypoxia), hypothermia, hypotension, or electrolyte imbalance.
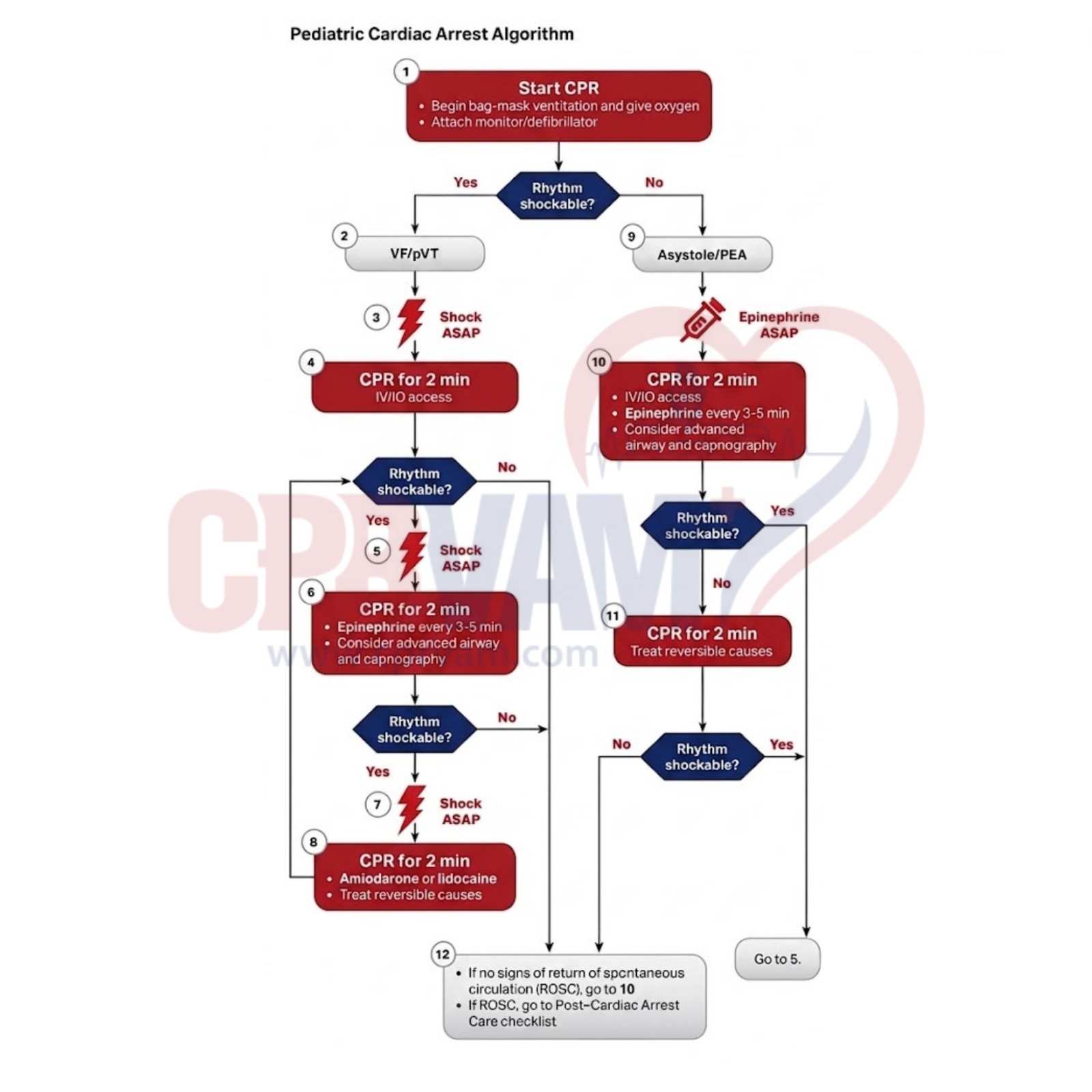
The Pediatric Cardiac Arrest Algorithm is a clear, step-by-step guide to help healthcare providers treat children whose hearts have stopped or are beating dangerously. It focuses on checking the child’s airway, breathing, and circulation, performing high-quality CPR, using an AED when needed, and giving medicines to improve chances of survival.
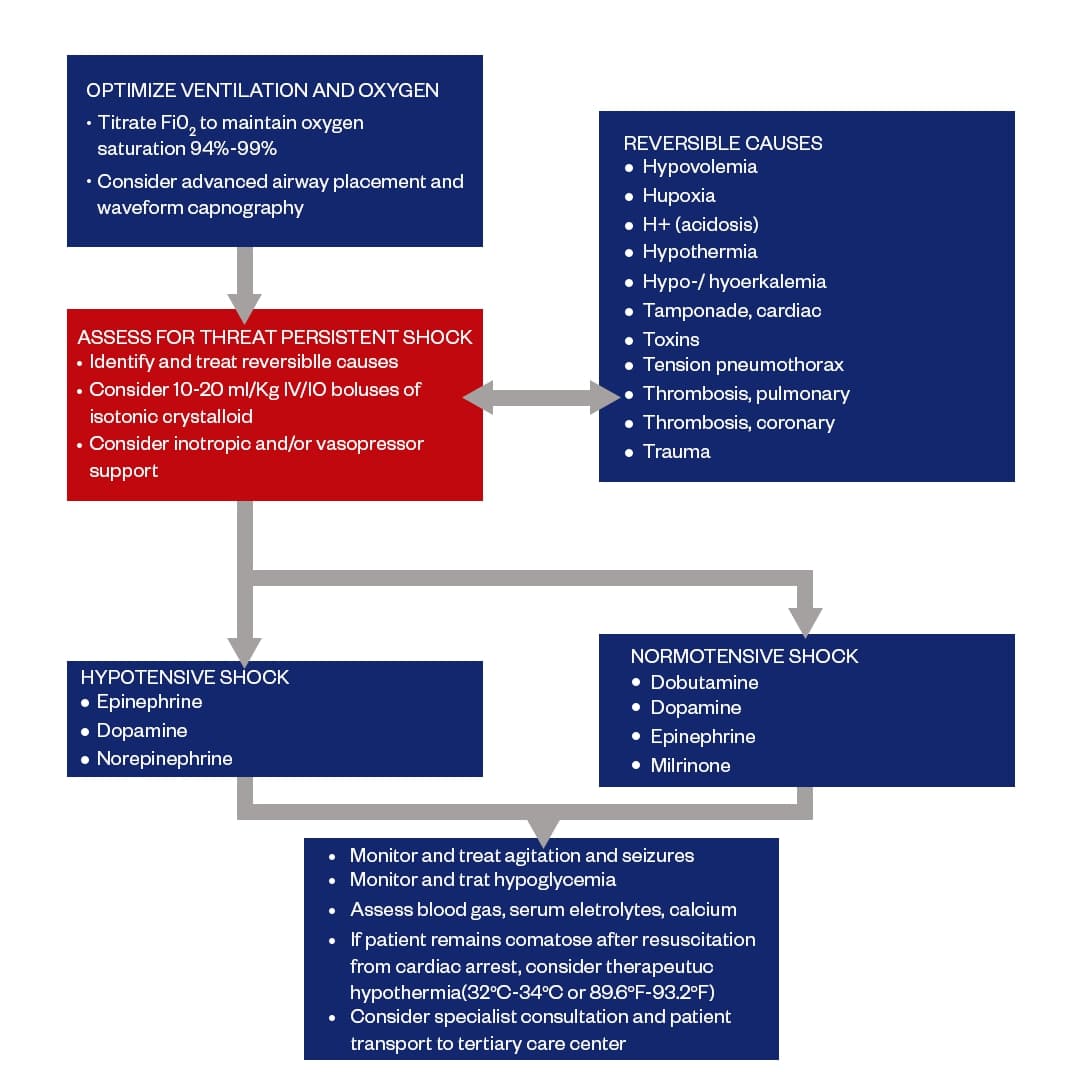
Return of spontaneous circulation (ROSC) in the pediatric patient, a phase called post-resuscitation care starts, which requires more intensive and integrated care. A systematic and coordinated approach, called the Pediatric post-resuscitation care algorithm, has been introduced to facilitate this care.
The PALS algorithm is essential in pediatric emergencies because it provides a structured, evidence-based approach for early recognition and treatment of life-threatening conditions. It improves decision-making, reduces errors, and increases survival by guiding systematic assessment and timely intervention in critically ill infants and children.
Systematic Emergency Approach
PALS offers a clear step-by-step process to manage pediatric emergencies like cardiac arrest, bradycardia, and tachycardia effectively.
Early Recognition of Deterioration
It helps clinicians quickly identify respiratory distress or shock before they progress into cardiac arrest.
Pediatric-Specific Care
The algorithm ensures correct drug dosing, equipment selection, and care based on child-specific physiology.
Effective Team Coordination
PALS promotes clear roles and communication among the resuscitation team during high-pressure situations.
Post-Resuscitation Care
It guides stabilization after ROSC to maintain organ function and prevent secondary complications.
The PALS algorithm uses a tiered assessment model. It ensures systematic evaluation of pediatric patients. This approach helps identify life-threatening conditions quickly and guides timely, effective clinical interventions.
The PAT is a rapid, hands-off assessment used to quickly evaluate a child’s overall condition. It helps identify respiratory, circulatory, or neurological distress within seconds of first contact.
The ABCDE approach systematically identifies life-threatening problems by evaluating airway, breathing, circulation, neurological status, and exposure in a structured and prioritized sequence.
The SAMPLE history is used after stabilization to gather focused clinical information that supports diagnosis and helps guide ongoing treatment decisions in pediatric care.
The 2025 AHA PALS updates improve early recognition of patient deterioration. They strengthen CPR quality and airway management. They also enhance teamwork and coordination during pediatric emergencies.
Here are the key updates to the PALS algorithm:
Rhythm-based management in PALS directs treatment based on cardiac rhythm type. It guides defibrillation, medication timing, and continuous CPR, ensuring an organized and effective response during pediatric cardiac arrest situations.
Advanced airway management in PALS 2025 follows a structured, stepwise approach beginning with basic ventilation and progressing to advanced airway techniques when clinically required. It emphasizes maintaining oxygenation and circulation while minimizing interruptions in chest compressions during pediatric resuscitation.
Key Highlights
The PALS algorithm is implemented in clinical practice through structured systems, tools, and training programs. These measures ensure accurate dosing, rapid decision-making, coordinated team response, and reduced errors, ultimately improving the quality and outcomes of pediatric emergency care.
Key Points:
The PALS algorithm is used in pediatric emergencies when a child shows life-threatening conditions such as cardiac arrest, respiratory compromise, shock, arrhythmias, or rapid clinical deterioration requiring immediate structured resuscitation and intervention.
Key Indications:
The latest AHA updates improve pediatric emergency care by focusing on practical, evidence-based resuscitation methods. They highlight the importance of early recognition of deterioration and quick intervention. High-quality CPR, better airway management, and rhythm-based care are central to the approach. Together, these changes help improve survival and long-term brain outcomes in children.
Healthcare professionals are encouraged to fully understand and apply the PALS algorithm in real emergencies. Proper training helps them respond quickly and work effectively as a team during critical situations. The CPR VAM Training Center provides structured BLS, ACLS, and PALS courses. With expert instructors and hands-on practice, learners build strong clinical skills and confidence.
It provides a structured method for rapidly assessing and treating critically ill children. This helps clinicians make timely decisions and deliver effective life-saving care.
It organizes care into clear steps, allowing faster identification of critical conditions. This reduces delays and improves coordination among healthcare providers.
Children have different physiologies, requiring age-appropriate dosing and equipment. This approach reduces errors and improves safety during emergency treatment.
Clear role assignment and communication ensure smooth coordination during high-pressure events. This improves efficiency and reduces confusion during critical interventions.
Regular hands-on practice builds confidence and clinical skills for real situations. It helps healthcare providers respond quickly and accurately during emergencies.


