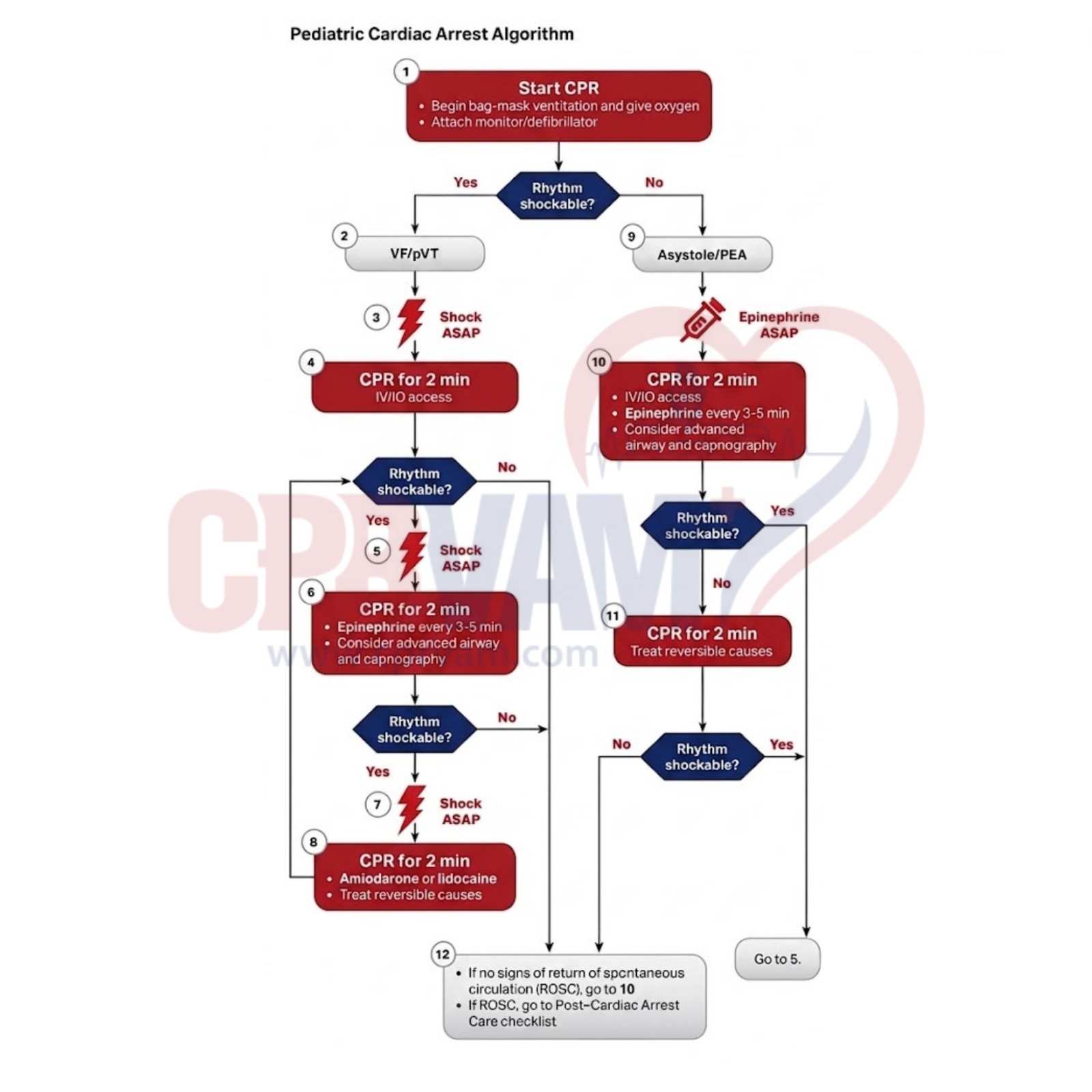
Post–Cardiac Arrest Care in Pediatric Patients (After ROSC)
Post-resuscitation care begins immediately after return of spontaneous circulation (ROSC) and focuses on stabilizing the child and preventing further organ damage. The goal is to support heart, brain, and lung function while addressing the underlying cause of arrest.
Key Management Steps:
- Ensure adequate oxygenation and controlled ventilation
- Maintain normal blood pressure and treat hypotension promptly
- Monitor heart rhythm and hemodynamic status continuously
- Manage body temperature to protect brain function
- Identify and treat the underlying cause of cardiac arrest
- Prepare for intensive care transfer and ongoing monitoring