- 2026
CPR VAM • All Rights Reserved • Developed by Splendour Group

Basic Life Support (BLS) is a vital, life-saving protocol for managing cardiac arrest and other emergencies. The 2025 American Heart Association (AHA) BLS Algorithm provides healthcare providers with a structured, step-by-step guide to quickly recognize emergencies, activate help, and deliver high-quality CPR and defibrillation. Designed for both lone rescuers and teams, it ensures organized, effective care that maintains circulation and oxygenation, improving survival chances.
The BLS Algorithm offers clear pathways for adults and children, including guidance for different clinical scenarios. It helps doctors, nurses, EMTs, and lifeguards identify the cause of cardiac arrest quickly and provide precise, life-saving interventions. Following this evidence-based protocol sustains vital functions, restores circulation, and aligns emergency responses with the latest AHA guidelines, giving patients the best chance to survive critical events.

BLS algorithms are essential for guiding responders during emergencies, offering a clear, step-by-step approach that ensures quick, accurate, and coordinated interventions, ultimately improving patient outcomes and saving lives.
Here are the importance of BLS Algorithms in emergency care as follows:
Standardized Emergency Care
BLS algorithms establish a consistent and structured approach to emergency response, ensuring uniform and high-quality care across all healthcare settings.
Improved Patient Survival Rates
The proper application of BLS algorithms enhances patient survival by enabling timely CPR, effective ventilation, and rapid defibrillation to maintain circulation and oxygenation.
Faster and Accurate Decision-Making
BLS algorithms support prompt and precise decision-making by providing clear, step-by-step guidance during critical emergencies.
Enhanced Team Coordination and Efficiency
BLS algorithms promote effective teamwork by defining roles and improving communication, allowing responders to coordinate efficiently and minimize delays.
Confidence and Skill Development for Responders
Consistent use of BLS algorithms strengthens essential life-saving skills and builds responder confidence to act decisively and effectively in emergencies.
Maintaining BLS certification equips these professionals with the knowledge and skills to deliver high-quality CPR, operate an AED, and follow structured emergency protocols. This training not only improves patient survival rates but also ensures care aligns with the latest AHA evidence-based guidelines.
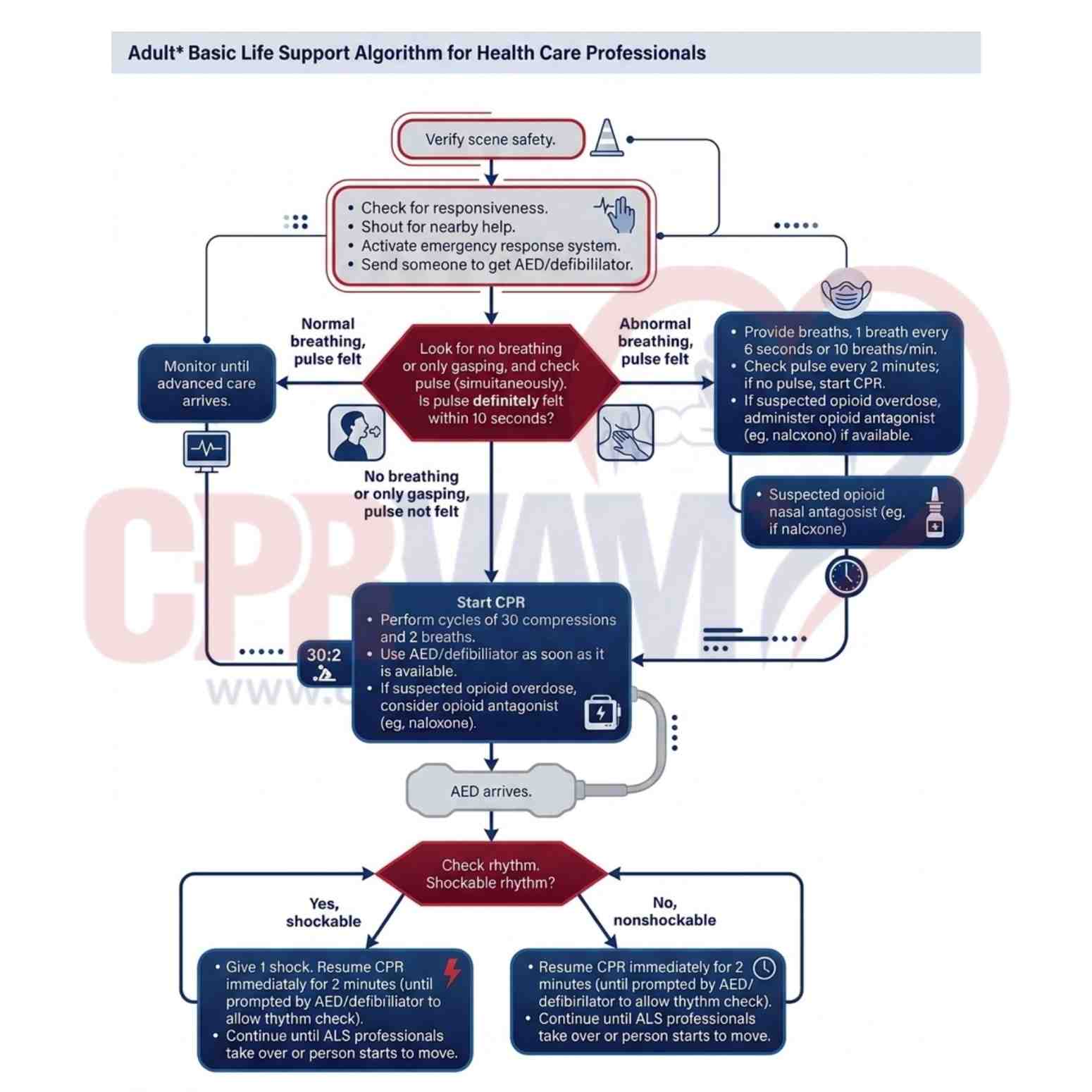
Adult Basic Life Support (BLS) saves lives during cardiac arrest, respiratory failure, choking, drowning, or trauma. Follow 2025 AHA guidelines: assess responsiveness, start CPR, provide rescue breaths, use an AED, and call for help. Avoid BLS if breathing, unsafe scene, obvious death, or DNR orders. Correct technique ensures effective resuscitation.
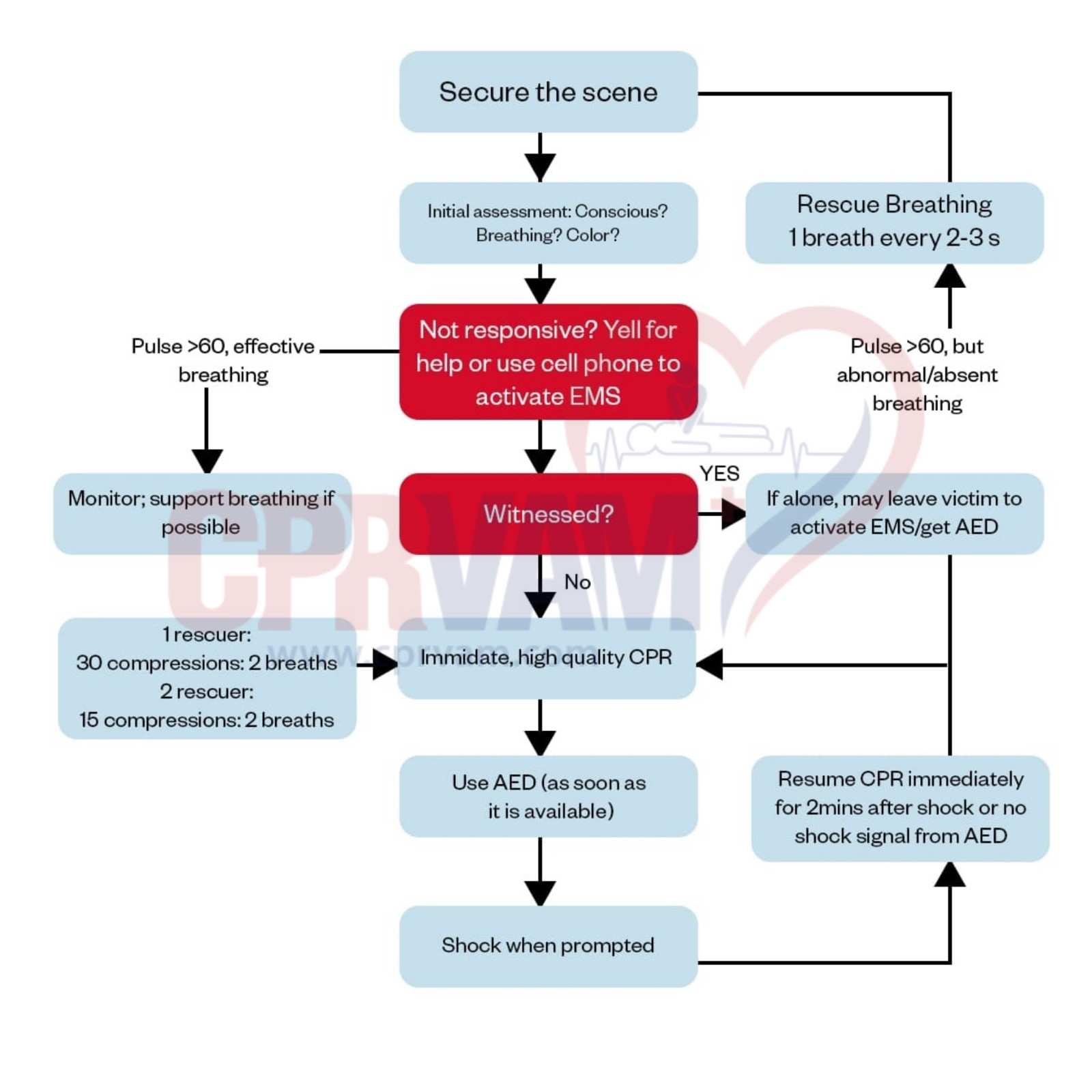
Pediatric BLS saves infants and children during cardiac arrest, drowning, choking, or emergencies. Follow ILCOR guidelines: ensure scene safety, assess responsiveness, activate help, perform high-quality chest compressions, give rescue breaths, and use an AED when needed. Single- or two-rescuer approaches ensure continuous care until advanced medical support arrives.
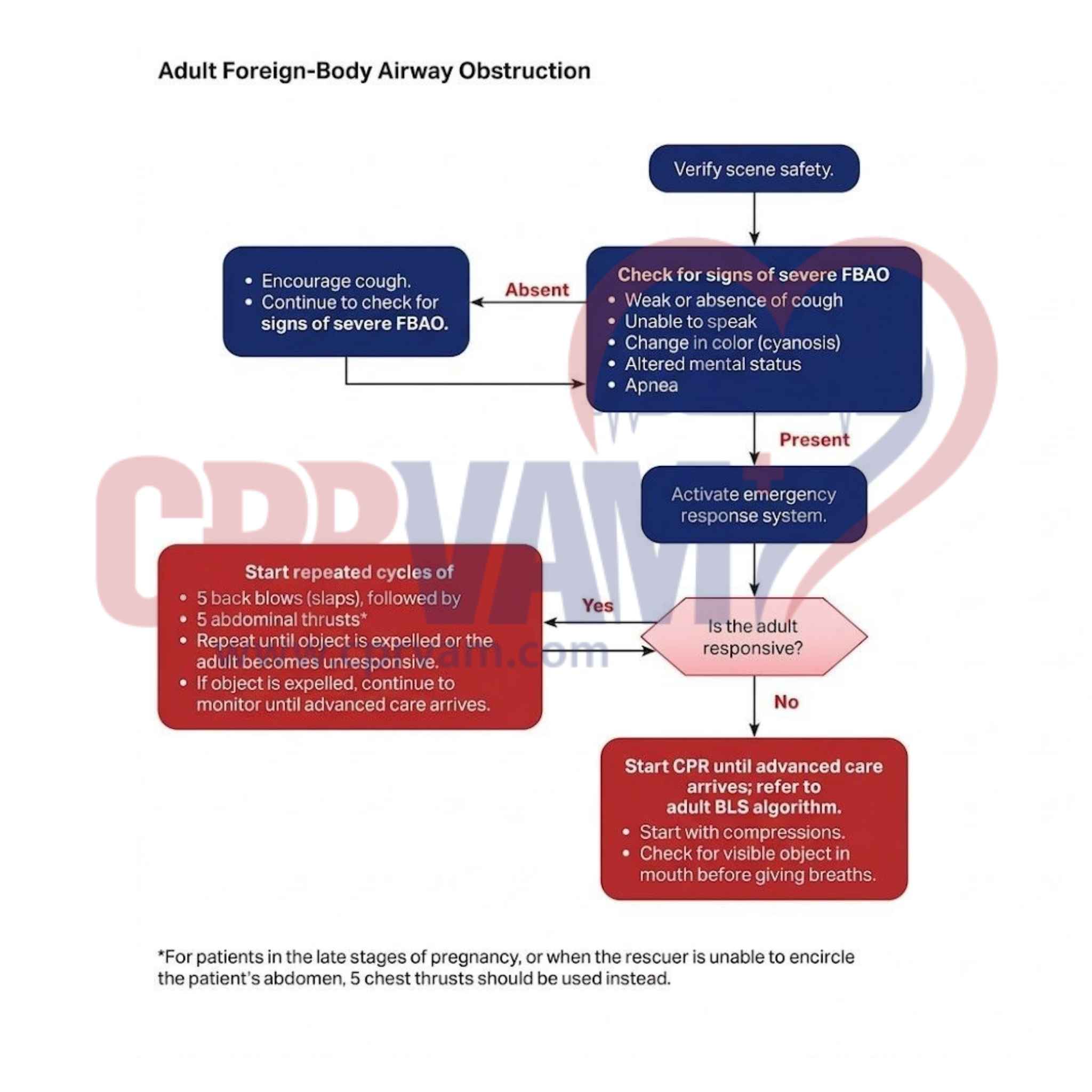
The 2025 AHA Adult Choking Algorithm guides responders to quickly assess airway obstruction, provide back blows, abdominal or chest thrusts, and escalate to CPR if unresponsive. Ensuring scene safety, calling for help, and following stepwise interventions improves survival. Applicable to healthcare providers, first responders, and trained bystanders.
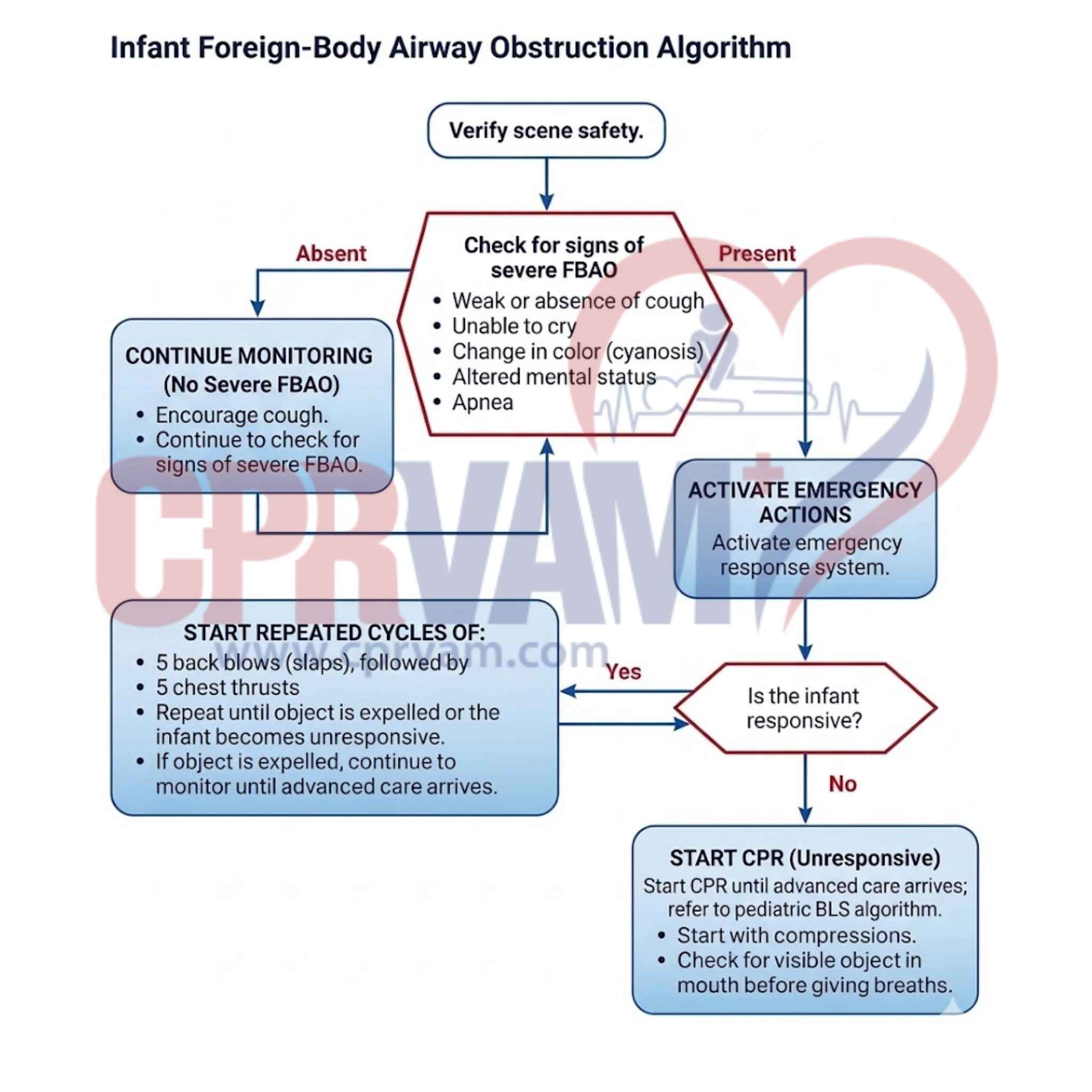
The 2025 Infant FBAO Algorithm guides caregivers and responders to act quickly when infants choke. Recognize signs, perform five back blows and chest thrusts, monitor responses, and start CPR if unresponsive. Following this step-by-step, evidence-based approach ensures safe, confident action, improving survival and reducing complications in airway emergencies.
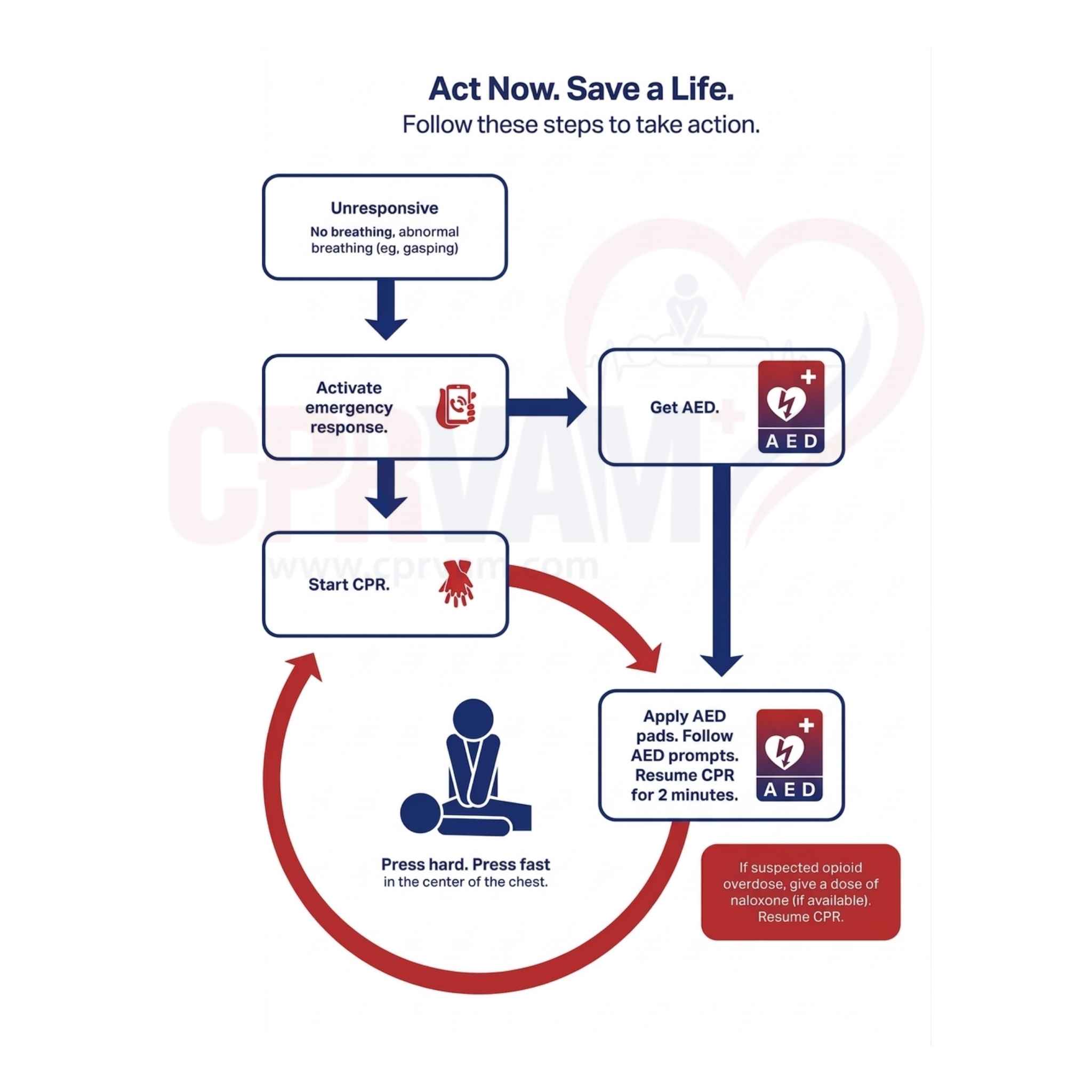
Adult BLS empowers lay rescuers to respond to cardiac emergencies. Quickly assess responsiveness, call for help, start high-quality chest compressions, provide rescue breaths if trained, and use an AED promptly. Following these steps boosts survival, builds confidence, and ensures safe, effective intervention until professional help arrives.
Maintaining proficiency in Basic Life Support requires continuous practice, realistic training, effective teamwork, and staying updated with evolving guidelines to ensure accurate, confident, and timely response during emergencies.
Regular Practice
Regular practice of BLS steps strengthens muscle memory, improves response time, and ensures accurate performance of life-saving techniques during real emergencies.
Simulation Training
Simulation training allows responders to apply BLS algorithms in realistic scenarios, enhancing critical thinking and building confidence in emergency management.
Team Coordination
Understanding team roles and responsibilities improves communication and coordination, ensuring efficient and error-free execution of BLS procedures.
Stay Updated
Staying updated with the latest BLS guidelines ensures that responders follow current, evidence-based practices for effective and compliant emergency care.
Basic Life Support (BLS) is used during sudden life-threatening emergencies that stop breathing or circulation. Immediate action by trained responders, using CPR, rescue breaths, and defibrillation, helps maintain vital functions until advanced medical care arrives.
Common situations requiring BLS include:
Adult Cardiac Arrest Management
The heart stops beating, leaving the person unresponsive with abnormal breathing and no pulse. Immediate CPR and AED use are critical.
Pediatric Emergency Response
Children usually experience arrest from respiratory failure, so BLS must support both breathing and circulation.
Respiratory Arrest Intervention
Breathing stops while the heart is still beating. Rescue breaths are prioritized to prevent cardiac arrest.
Drowning Emergency Care
Water in the airway causes oxygen loss. Begin BLS with five rescue breaths, then CPR.
Choking and Airway Obstruction Management
Blocked airways require back blows and abdominal thrusts; BLS starts if unresponsiveness occurs.
Opioid Overdose Response
Respiratory suppression from opioids may lead to arrest. BLS, alongside naloxone administration, restores breathing and circulation.
BLS certification is essential for many healthcare and safety professionals. Understanding the BLS Algorithm ensures these individuals can respond quickly and effectively during life-threatening emergencies. The American Heart Association (AHA) requires certain roles to maintain current certification to provide safe, standardized care in hospitals, clinics, and community settings.
Professionals commonly required to hold BLS certification include:
The 2025 BLS algorithm introduces significant changes to improve patient outcomes. It includes updated CPR guidelines for adults and children, adjustments for pregnant patients, trauma and spinal care, drowning management, and opioid overdose response. These updates ensure timely, effective, and life-saving interventions in all healthcare settings.
BLS techniques vary by age and size. Adults need deeper, two-hand compressions, while children and infants require gentler methods. Pediatric cases prioritize rescue breaths due to respiratory causes, ensuring safe, effective care.
Pregnant patients require adjusted hand placement and left uterine displacement to improve circulation. Slight positioning changes protect mother and baby, while uninterrupted, high-quality chest compressions remain essential for maintaining oxygenation and survival.
Trauma cases require spinal stabilization while delivering continuous chest compressions. Control severe bleeding and maintain alignment of the head, neck, and spine. Effective BLS ensures life-saving care while reducing the risk of further injury.
Drowning cases require immediate oxygenation. Start with rescue breaths before chest compressions, remove the victim safely from water, and activate emergency services. Early ventilation and timely intervention significantly improve survival outcomes.
Opioid overdoses cause respiratory depression, leading to cardiac arrest. Administer naloxone quickly using proper routes, continue CPR with rescue breaths, and ensure rapid emergency response. Consistent BLS care improves oxygenation and increases the chances of survival.
Key Aspect | Single Rescuer BLS | Two Rescuer BLS |
Rescuer Roles | One person performs all tasks, including compressions, rescue breaths, and AED operation | Tasks are shared: one performs compressions while the other manages airway, rescue breaths, and AED |
Compression-to-Breath Ratio | 30 compressions followed by 2 rescue breaths for all ages | 30:2 for adults; 15 compressions followed by 2 breaths for infants and children |
Emergency Call / EMS Activation | CPR must be paused to call emergency services | One rescuer continues CPR while the other calls EMS, ensuring uninterrupted care |
Task Management & Coordination | All responsibilities handled by one rescuer, which may reduce efficiency | Role division allows smoother workflow, better quality compressions, and faster interventions |
Fatigue and Role Rotation | High risk of fatigue due to continuous activity | Rescuers switch roles every 2 minutes to maintain high-quality compressions and reduce |
The Basic Life Support (BLS) Algorithm is a structured, evidence-based framework for managing life-threatening emergencies.It emphasizes early recognition of unresponsive victims, high-quality chest compressions, effective rescue breaths, and rapid use of an automated external defibrillator (AED). Timely, precise interventions significantly improve survival and recovery outcomes. Healthcare providers and individuals can enhance their skills through RQI-approved AHA BLS Certification at CPR VAM Training Center, gaining comprehensive, life-saving knowledge and confidence.
The Basic Life Support (BLS) Algorithm is a step-by-step approach for recognizing and responding to life-threatening emergencies, such as cardiac arrest or respiratory failure. It guides rescuers on checking responsiveness, performing chest compressions, providing rescue breaths, and using an AED.
The recommended compression rate for adults is 100–120 per minute with a depth of 5–6 cm (2–2.5 inches). For children, compressions should also be 100–120 per minute, reaching approximately one-third of the chest depth (about 5 cm or 2 inches). Infants require the same rate (100–120 per minute) with a depth of about 4 cm (1.5 inches). Always ensure the chest fully recoils after each compression to optimize blood flow and improve the effectiveness of CPR.
If a choking child becomes unresponsive, call for help and start CPR. Begin 30 chest compressions at the center of the chest, then give 2 rescue breaths. Each time you open the airway, check for any visible obstruction and remove it only if you can see it. Continue cycles of compressions and breaths until the child starts breathing, coughs, or professional help arrives.
The sniffing position is a head and neck alignment used to open a child’s airway during resuscitation. To achieve it, tilt the head slightly back and lift the chin, as if the child is “sniffing the air.” This position helps keep the airway open for effective rescue breaths or ventilation while minimizing neck strain.
In one-person CPR, perform 30 chest compressions followed by 2 rescue breaths. In two-person CPR, one compresses while the other breathes, switching roles every two minutes to prevent rescuer fatigue.


