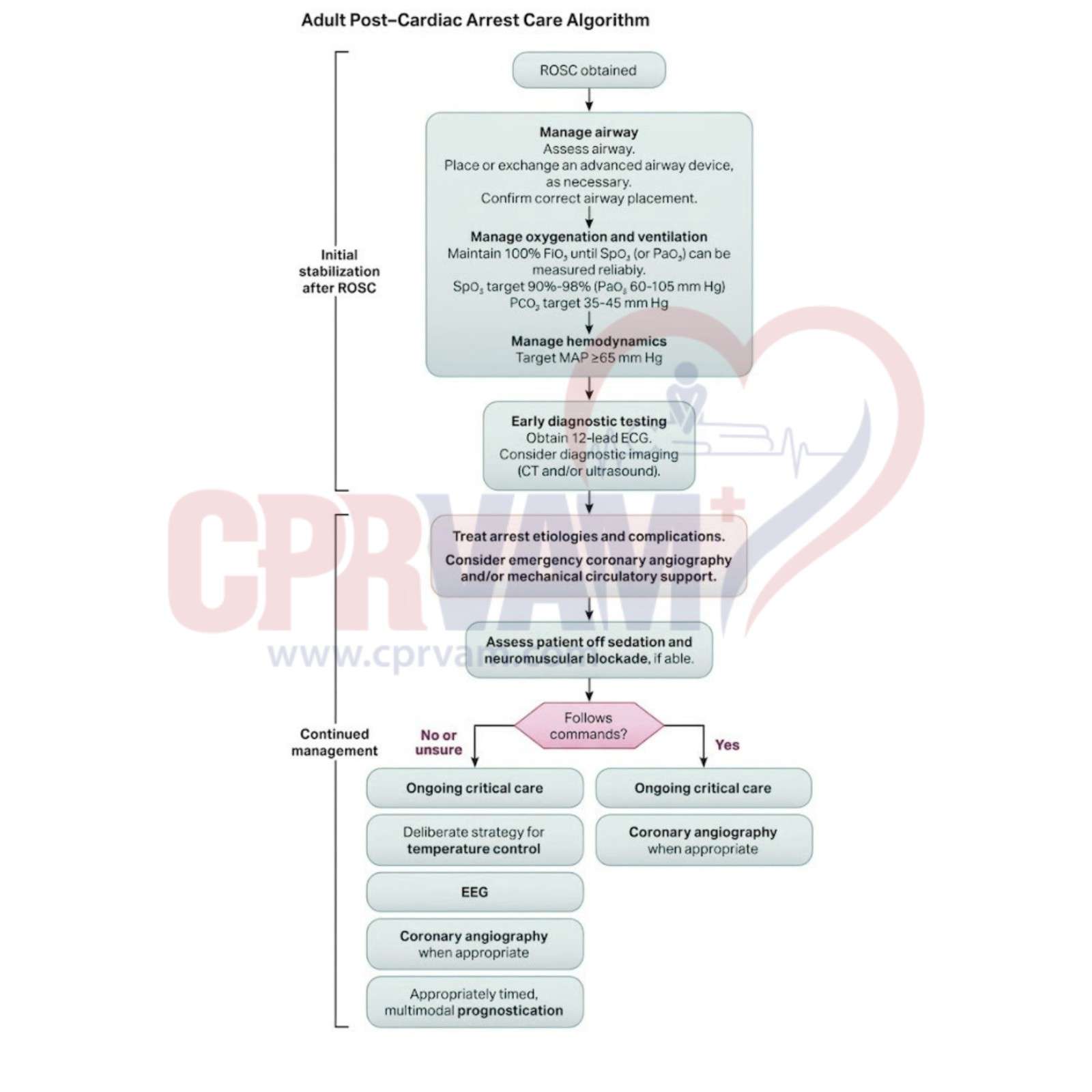
Importance of the Adult Post–Cardiac Arrest Care Algorithm
The Adult Post–Cardiac Arrest Care Algorithm provides a structured approach after ROSC. It ensures rapid stabilization, brain protection, and timely treatment to improve survival and neurological recovery.
Provides a Clear Step-by-Step Clinical Framework
It gives healthcare teams a structured sequence of actions after cardiac arrest. This reduces confusion and ensures faster, more organized decision-making in critical situations.
Ensures Immediate Physiological Stabilization
The algorithm prioritizes airway, breathing, circulation, and oxygen delivery. This helps stabilize vital organs, especially the brain and heart, in the first hours after ROSC.
Prevents Secondary Complications After ROSC
It helps avoid complications like low oxygen, low blood pressure, and recurrent arrest. Continuous monitoring reduces preventable deterioration after initial resuscitation.
Supports Timely Diagnosis and Treatment of the Cause
The algorithm encourages early testing, such as ECG and imaging, to find the cause of arrest. Treating the underlying problem helps prevent recurrence and improves outcomes.
Protects the Brain and Improves Neurological Outcomes
It includes strategies like temperature control and EEG monitoring. These steps reduce brain injury and increase the chances of meaningful neurological recovery.
Standardizes High-Quality Critical Care
It ensures all patients receive consistent, evidence-based care regardless of location. This improves teamwork, reduces errors, and enhances overall treatment quality.
Improves Survival and Long-Term Recovery Outcomes
Structured post-arrest care increases survival rates and improves brain function recovery. It also supports better long-term health and rehabilitation outcomes.