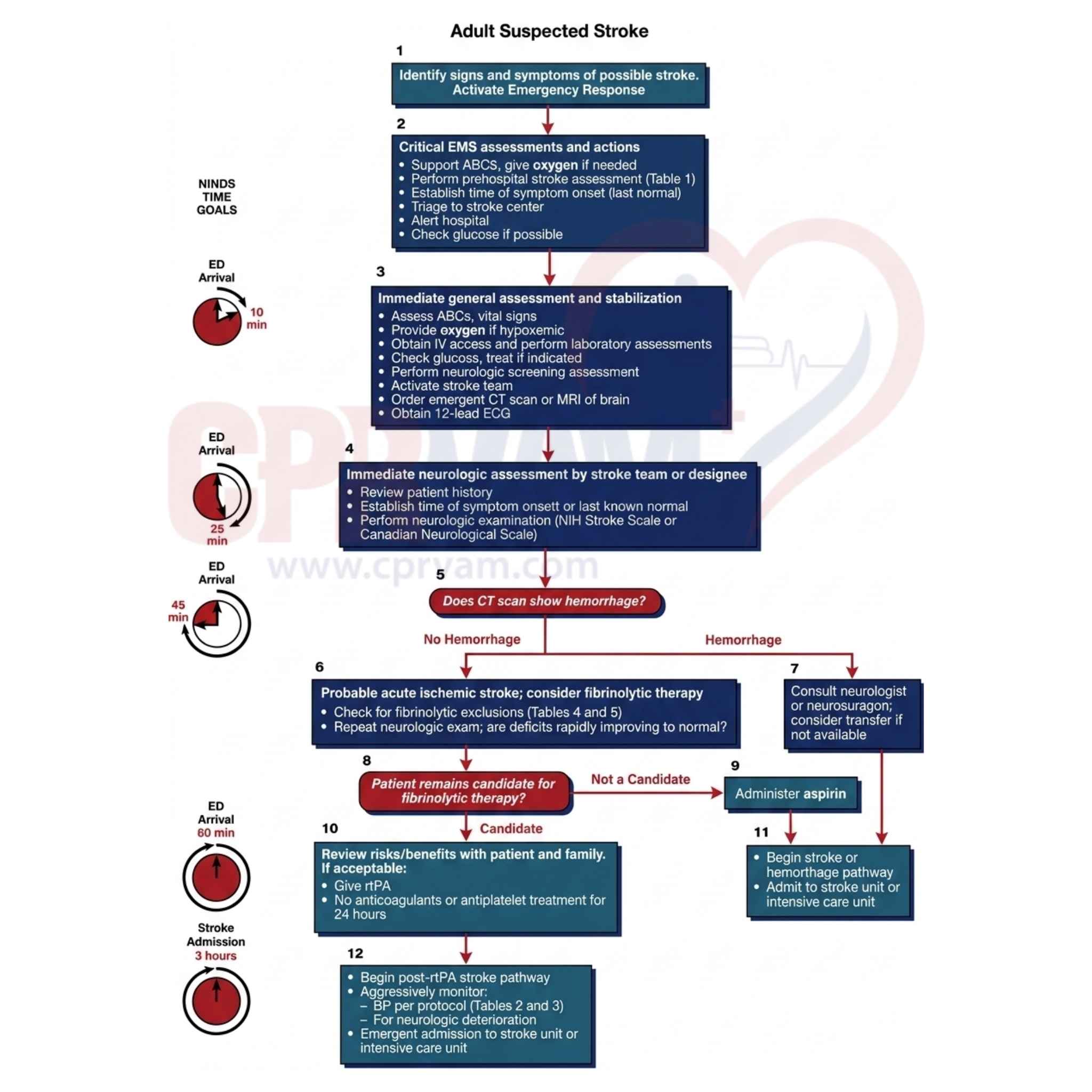
Time Matters: Key Takeaways from the Adult Suspected Stroke Algorithm
The Adult Suspected Stroke Algorithm is a vital emergency guide that helps healthcare providers act quickly when stroke is suspected. It ensures early recognition, rapid response, and timely treatment to protect brain function, improve survival, and reduce long-term disability.
At the CPR VAM Training Center, you will learn these algorithms through practical, hands-on training based on AHA guidelines. The course builds confidence in emergency response, helping you apply stroke management steps effectively in real-life clinical situations when every second matters.