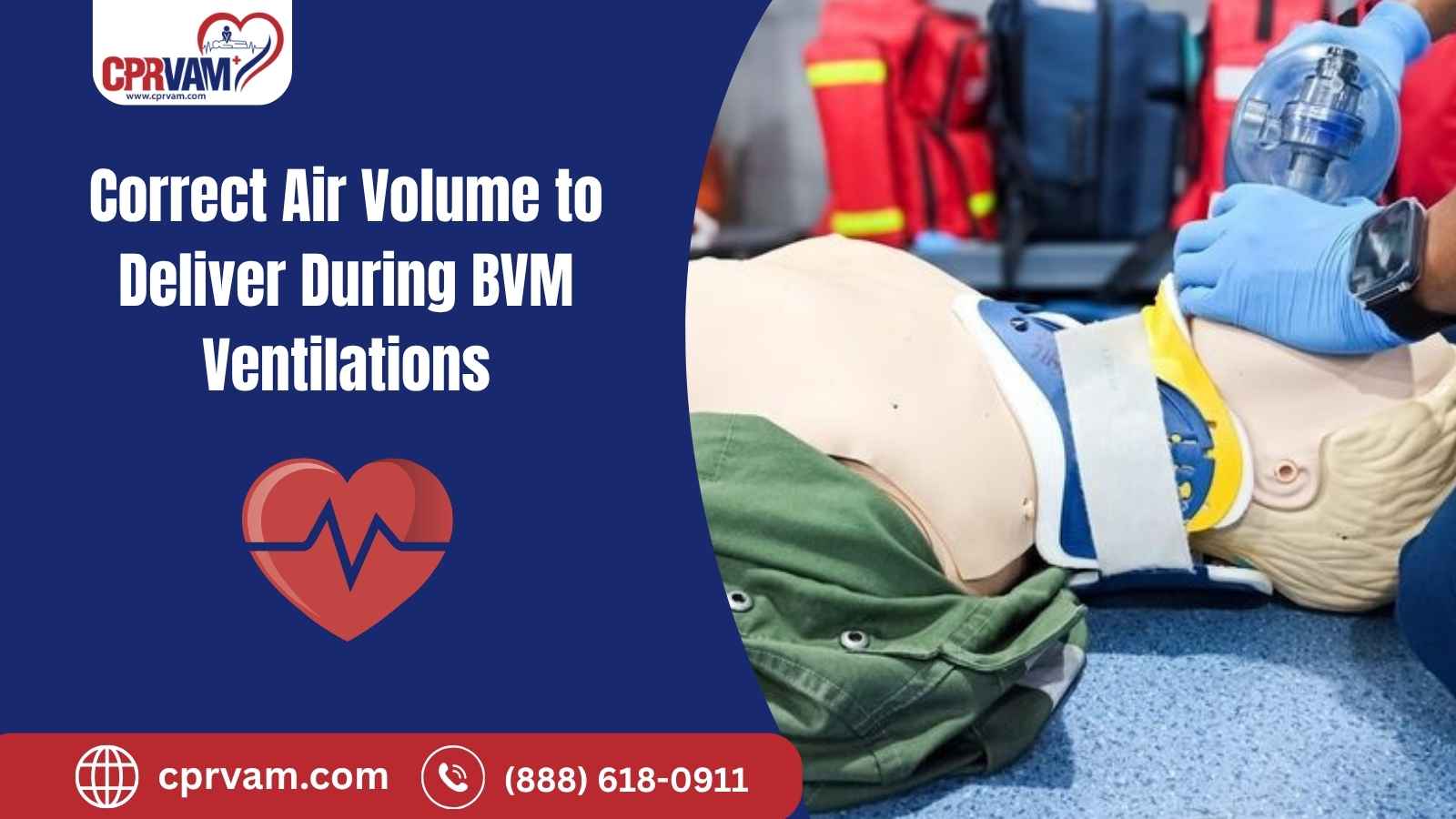
Imagine being in an emergency where every second counts, and someone’s life depends on the air you deliver. Bag-Valve-Mask (BVM) ventilation is a vital skill in those moments, helping patients breathe when they can’t on their own. But delivering the right amount of air is not as simple as it seems. Too little can starve organs of oxygen, while too much can harm the lungs or stomach.
Understanding the correct volume of air during BVM ventilations is essential for anyone providing emergency care. Whether you are performing CPR, assisting a trauma patient, or helping someone with severe respiratory failure, knowing how much air to deliver keeps the patient safe and improves their chances of recovery.
This blog guides you through practical, evidence-based techniques that follow American Heart Association guidelines.
Why Correct Air Volume Matters in BVM Ventilation?
Delivering the correct air volume during Bag-Valve-Mask (BVM) ventilation is one of the most important skills in emergency care. Getting it right ensures your patient receives enough oxygen to vital organs while avoiding lung injury, gastric inflation, or reduced cardiac output. As a rescuer, knowing how much air to deliver can directly impact survival during CPR or respiratory emergencies.
Oxygen Delivery to the Brain and Heart: Proper ventilation ensures vital organs get the oxygen they need to function.
Removal of Carbon Dioxide: Adequate breaths help your patient eliminate CO₂ efficiently, preventing acidosis.
Intrathoracic Pressure and Cardiac Output During CPR: Over-ventilating can reduce blood flow to the heart and brain.
Risk of Ventilation-Related Complications: Delivering too much or too little air increases the chances of lung injury, aspiration, or stomach inflation.
According to the American Heart Association, over-ventilating during CPR is a common mistake that can harm patients. The key is to take controlled breaths that cause a gentle, visible rise in the chest.
How Do You Measure and Deliver the Right Tidal Volume During BVM Ventilation?
Tidal volume is the amount of air pushed into the lungs with each breath during BVM ventilation. Delivering the right amount is crucial. You want to give enough air to oxygenate organs without causing lung injury. As a rescuer, observing the patient helps you get it just right every time.
Visible Chest Rise: Watch the chest gently lift with each breath. This is the clearest sign that air is entering the lungs effectively.
Patient Size and Age: Adjust the volume based on whether you are helping an adult, child, or infant. Their lungs differ, and you need to match their needs.
Clinical Response: Check oxygen saturation, end-tidal CO₂, and breath sounds to see if your patient is receiving proper ventilation. These signs guide you to adjust the tidal volume safely.
Delivering the correct tidal volume during BVM ventilation ensures your patient gets enough oxygen while preventing lung injury. Watching chest rise, adjusting for age and size, and monitoring vital signs helps you provide safe, effective breaths every time.
What Is the Correct Air Volume for BVM Ventilation?
Delivering the right air volume during Bag-Valve-Mask ventilation is crucial for effective resuscitation. Giving too little air can deprive vital organs of oxygen, while too much can cause lung injury or stomach inflation. When you are providing ventilation, knowing how much air to deliver ensures your patient gets safe, effective breaths every time.
For adults, the safe and recommended air volume during BVM ventilation is typically 500-600 milliliters per breath.
Pediatric patients require smaller tidal volumes than adults. Infants under 1 year should receive 20-30 milliliters per kilogram of body weight, while children aged 1 to 8 years need 10-15 milliliters per kilogram.
Using this air volume helps you provide effective ventilation while protecting the lungs and stomach and keeping blood flow steady during CPR.
Overview of Pediatric Patients and Weight-Based Ventilation
Patient Group | Recommended Volume per Breath |
Infants (< 1 year) | 20-30 mL/kg |
Children (1-8 years) | 10-15 mL/kg |
Adolescents | Same as adults (500-600 mL) |
Children are particularly susceptible to over-ventilation, making precise control of tidal volume essential for safe and effective ventilation.
How Do You Accurately Assess the Correct BVM Ventilation Volume?
Getting the right air volume during BVM ventilation can be tricky, but it’s one of the most important skills you can master. Deliver too little, and vital organs may go without oxygen. Deliver too much, and you risk lung injury. By watching key signs, you can make sure every breath you give is safe and effective.
Gentle, Visible Chest Rise: Watch the chest lift softly with each breath. This shows you that air is entering the lungs effectively without overinflation.
Stable or Improving Oxygen Saturation (SpO₂): Monitor the patient’s oxygen levels. If SpO₂ remains steady or improves, you know your ventilation is adequate.
Appropriate End-Tidal CO₂ Values: Checking CO₂ levels helps you see if the patient is ventilating properly. You can adjust the volume based on these readings.
Equal Bilateral Breath Sounds: Listen to both lungs to ensure air is reaching them evenly. Unequal sounds may indicate improper mask placement or inadequate volume.
Warning Signs: Forceful or exaggerated chest rise usually means you are delivering too much air. You should adjust to maintain safe, effective ventilation.
What Are the Best Techniques for Delivering the Correct BVM Ventilation Volume?
Delivering the correct BVM ventilation volume is critical for effective oxygenation and patient safety. When you use proper techniques, you can ensure each breath is adequate, consistent, and gentle. Mastering these methods helps you minimize complications like lung injury, gastric inflation, and poor circulation during resuscitation.
1. Two-Handed Mask Seal
When you work with a partner, using a two-handed mask seal provides the best control. One person maintains a tight seal with both hands while you squeeze the bag. This technique helps you deliver consistent breaths and reduces the risk of air leaks during ventilation.
2. One-Handed Technique
If you are alone, the one-handed technique allows you to hold the mask and squeeze the bag simultaneously. While convenient, you must be aware that this method carries a higher risk of an inadequate seal and uneven ventilation.
Technique Principles (Additional Tips)
To deliver effective breaths, you should give each breath slowly over about one second. Allow the chest to fully recoil between breaths, and avoid forceful or rapid bag compression. Following these principles helps you maintain safe, controlled ventilation for every patient.
What Are the Risks of Incorrect BVM Ventilation?
Even small mistakes in BVM ventilation can have serious consequences. Giving too much or too little air can compromise oxygen delivery, stress the heart, and damage the lungs. Knowing these risks helps you stay precise and keep your patient safe during resuscitation.
Here are the risks and potential consequences of incorrect BVM ventilation, presented in a clear table:
Errors/Risks | Potential Harm |
Hyperventilation | Reduced cerebral blood flow, decreased cardiac output |
Hypoventilation | Hypoxia, respiratory acidosis |
Gastric Insufflation | Vomiting, aspiration pneumonia |
Barotrauma | Lung injury, pneumothorax |
The majority of BVM-related complications arise from delivering excessive volume or rapid breaths, rather than from insufficient ventilation, highlighting the importance of controlled and precise technique.
Ensure Patient Safety: Apply Correct BVM Ventilation Techniques
Mastering BVM ventilation is not about squeezing the bag as hard as possible. It is about precision, control, and patient safety. Delivering the correct air volume, observing chest rise, and adjusting for age and size help protect the lungs, support circulation, and improve outcomes. Regular practice and careful technique make all the difference in emergencies. Take the time to refine your skills, follow evidence-based guidelines, and ensure every breath you deliver counts.
Ready to save lives with confidence? Master Bag-Valve-Mask ventilation and CPR training at CPR VAM, an AHA-approved training center. Learn the correct BVM air volumes, practice precise techniques, and ensure every breath you deliver is safe, controlled, and effective. Sign up today and become the rescuer who makes every second count.
FAQs
1. How Much Air Should You Actually Deliver With a BVM?
For adults, aim for 500-600 mL per breath, just enough for a gentle chest rise. Pediatric volumes are weight-based, making precise control essential for safe ventilation.
2. How Can You Tell If Your Breaths Are Effective?
Watch for a soft, visible chest rise, listen for clear breath sounds, and monitor oxygen saturation or CO₂ levels to ensure proper ventilation.
3. How Fast Should You Give Breaths During CPR?
Deliver about 10-12 breaths per minute for adults, or one breath every 5-6 seconds, following AHA guidelines to optimize oxygen delivery without over-ventilating.
4. Why Is Over-Ventilation Dangerous?
Too much air can reduce blood flow, damage lungs, and increase the risk of stomach inflation. Controlled, gentle breaths keep your patient safe.
5. Which Technique is Best for Effective BVM Ventilation?
Using a two-handed mask seal with a partner ensures consistent volume and reduces air leaks, while a one-handed approach works in emergencies but requires extra caution.