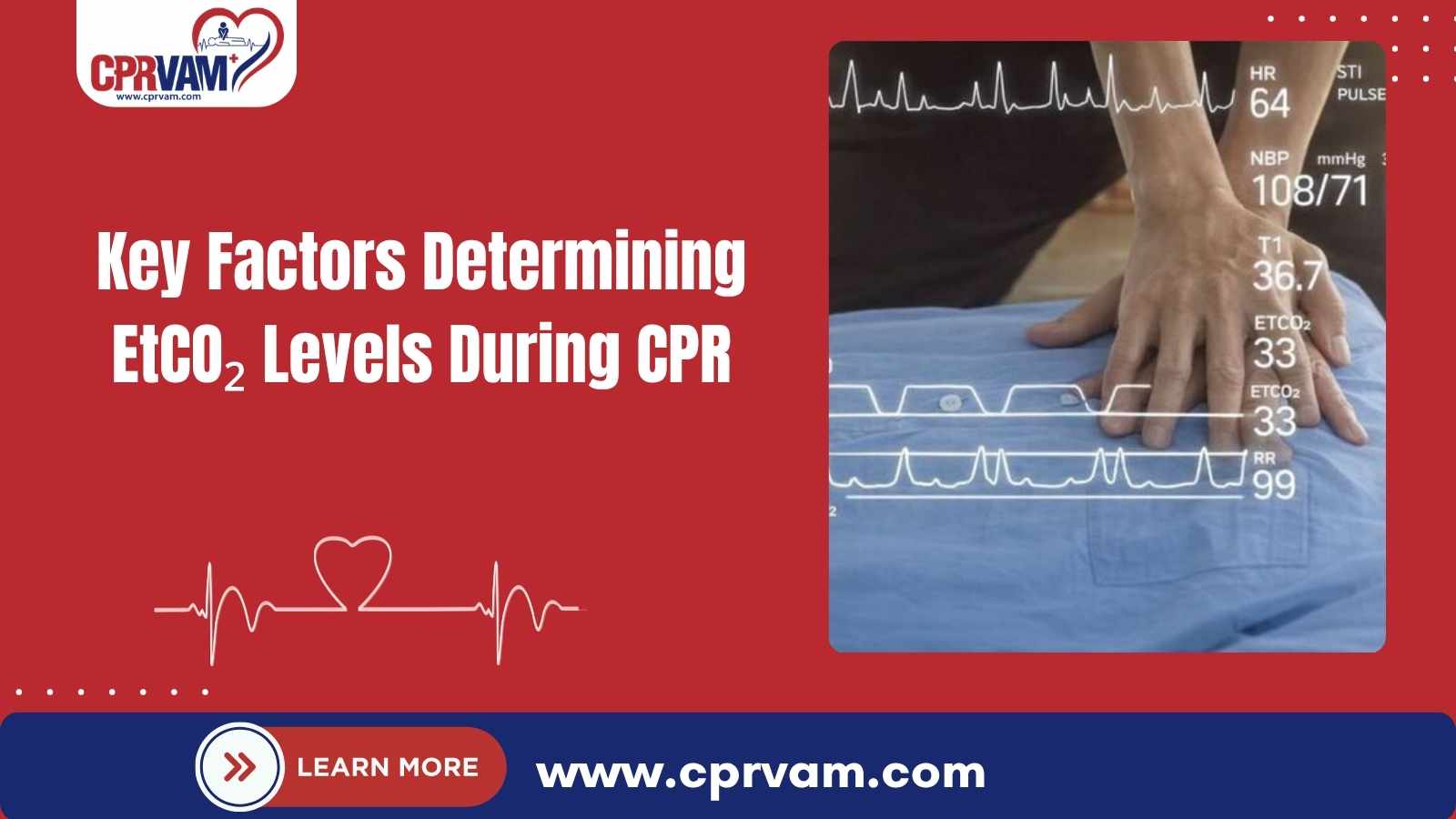
During cardiopulmonary resuscitation (CPR), every second matters, and rescuers need reliable, real-time indicators to assess whether their efforts are effectively supporting circulation. One of the most valuable tools used in modern resuscitation is end-tidal carbon dioxide (EtCO₂) monitoring. By measuring the amount of carbon dioxide exhaled at the end of each breath, EtCO₂ provides immediate insight into pulmonary blood flow and cardiac output during cardiac arrest.
EtCO₂ has become a critical component of high-quality CPR because it reflects how well chest compressions are generating circulation. Since carbon dioxide is transported from the tissues to the lungs through the bloodstream, EtCO₂ levels rise and fall in direct response to changes in blood flow. Higher readings suggest effective chest compressions and improved perfusion, while persistently low values signal inadequate circulation and the need to adjust resuscitation techniques.
This blog explains the main determinant of EtCO₂ during CPR, why chest compressions are key, and how EtCO₂ monitoring can guide rescuers to improve CPR quality and patient outcomes.
What Is EtCO₂ in CPR?
End-tidal carbon dioxide (EtCO₂) in CPR refers to the measurement of carbon dioxide concentration in exhaled air at the end of each breath using capnography. During cardiopulmonary resuscitation, EtCO₂ serves as a real-time, noninvasive indicator of pulmonary blood flow and cardiac output generated by chest compressions. In other words, EtCO₂ levels provide insight into the effectiveness of CPR.
EtCO₂ directly reflects circulation because carbon dioxide produced by the body’s tissues is transported to the lungs through blood flow. Higher EtCO₂ values indicate effective chest compressions and improved perfusion, while persistently low readings suggest poor compression quality or inadequate blood flow. In addition, EtCO₂ monitoring helps confirm proper airway placement and can detect return of spontaneous circulation (ROSC) even before a pulse is palpable.
What Is the Primary Factor That Influences EtCO₂ During CPR?
The primary factor that determines end-tidal carbon dioxide (EtCO₂) during CPR is the effectiveness of chest compressions, because they directly generate the blood flow that transports carbon dioxide from the tissues to the lungs. As compressions circulate blood, the body carries CO₂ produced by cellular metabolism to the lungs, and capnography measures it as EtCO₂. Consequently, the better the team performs compressions, including proper depth, rate, and full chest recoil, the higher the EtCO₂ levels.
Typically, rescuers interpret EtCO₂ values above 10-15 mmHg as evidence that compressions generate adequate circulation, whereas persistently low values indicate insufficient blood flow. When EtCO₂ remains low, it signals to the team that they must adjust compression technique, depth, or rate to improve perfusion. Because EtCO₂ responds almost immediately to changes in cardiac output, it provides a real-time, objective measure of CPR quality and guides clinical decisions throughout resuscitation.
What Are the Key Components of High-Quality Chest Compressions That Affect EtCO₂ During CPR?
Delivering high-quality chest compressions is essential for generating adequate blood flow during CPR, which directly impacts EtCO₂ levels and patient survival.
The main components of effective chest compressions include:
Compression Rate
Compressions should be delivered at 100–120 per minute. Maintaining this pace ensures continuous circulation without exhausting the rescuer too quickly.Compression Depth
For adults, compress at least 2 inches (5 cm) per compression. Adequate depth is necessary to create sufficient pressure to circulate blood effectively.Full Chest Recoil
Allow the chest to fully return to its normal position after each compression. This refill phase is critical for venous return and maintaining cardiac output.Minimal Interruptions
Reduce pauses in compressions as much as possible. Frequent interruptions significantly decrease blood flow and EtCO₂ levels.High Compression Fraction
Maximize the proportion of CPR time spent actively compressing the chest. Achieving a high compression fraction helps maintain circulation and improves resuscitation outcomes.
What Are Other Factors That Can Influence EtCO₂?
While chest compressions are the main determinant of EtCO₂ during CPR, several secondary factors can also affect readings. Understanding these influences is essential for accurately interpreting EtCO₂ trends and ensuring that resuscitation efforts are as effective as possible.
Here are some of the secondary factors that can influence EtCO2:
1. Ventilation Rate and Tidal Volume
The rate and volume of ventilation during CPR can significantly influence EtCO₂ readings. Over-ventilation, giving breaths too quickly or with excessive volume, can wash out carbon dioxide from the lungs, causing artificially low EtCO₂ values even if chest compressions are effective. Conversely, inadequate ventilation may fail to eliminate CO₂ properly.
2. Airway Placement and Patency
Proper airway placement and patency are essential for accurate EtCO₂ measurement during CPR. Incorrect placement, partial obstruction, or displacement of an airway device can reduce the amount of exhaled carbon dioxide, resulting in falsely low EtCO₂ readings.
3. Lung and Pulmonary Conditions
Lung and pulmonary health can significantly affect EtCO₂ readings during CPR. Conditions such as severe lung disease, pulmonary edema, or poor alveolar ventilation can impair the exchange of carbon dioxide, leading to lower EtCO₂ values even when chest compressions are adequate.
Monitoring and accounting for underlying pulmonary conditions helps ensure that EtCO₂ trends are interpreted correctly and that resuscitation efforts are adjusted appropriately.
4. Medications
Certain medications used during resuscitation can influence EtCO₂ readings by temporarily affecting circulation or pulmonary blood flow. For example, drugs that alter vascular tone or cardiac output may change how much CO₂ is transported to the lungs for exhalation.
5. Equipment Factors
Equipment issues can affect the accuracy of EtCO₂ readings during CPR. Faulty capnography sensors, leaks in the ventilation circuit, or moisture in the device can lead to incorrect measurements.
Regularly checking and maintaining all monitoring equipment ensures reliable EtCO₂ readings, allowing rescuers to assess circulation and the effectiveness of chest compressions accurately.
Why Is EtCO₂ Monitoring Clinically Important During CPR?
EtCO₂ monitoring is more than just a measurement; it provides critical, real-time feedback during resuscitation. By tracking exhaled carbon dioxide, healthcare providers can assess the effectiveness of chest compressions, detect changes in circulation, and make timely adjustments to improve patient outcomes.
Below are some of the importance of monitoring EtCO2:
1. Measures the quality of Chest Compressions
EtCO₂ directly reflects the cardiac output generated by chest compressions during CPR. Higher EtCO₂ values indicate effective compressions and adequate perfusion, while persistently low values suggest poor compression depth, rate, recoil, or frequent interruptions. Continuous monitoring allows immediate adjustment of compression quality without stopping CPR.
2. Early Detection of Return of Spontaneous Circulation (ROSC)
A sudden and sustained increase in EtCO₂ is an early indicator of ROSC. This rise often occurs before a palpable pulse or measurable blood pressure, allowing rapid recognition of spontaneous circulation and timely transition to post-cardiac arrest care.
3. Confirms Advanced Airway Placement
Continuous waveform capnography confirms correct tracheal placement of an advanced airway during CPR. A consistent EtCO₂ waveform indicates proper placement, while loss or reduction of the waveform may signal esophageal intubation, displacement, or obstruction.
4. Guides Ventilation and Prevents Hyperventilation
EtCO₂ monitoring helps regulate ventilation during CPR. Over-ventilation lowers EtCO₂ and reduces venous return and cardiac output. Monitoring EtCO₂ allows providers to adjust ventilation rate and volume to maintain adequate perfusion.
5. Provides Prognostic Information During Resuscitation
Persistently low EtCO₂ values despite high-quality CPR indicate poor circulation and a low likelihood of ROSC, while increasing EtCO₂ trends suggest improving perfusion. EtCO₂ should be used alongside other clinical findings, not as the sole determinant for resuscitation decisions.
Become a Confident Rescuer with Hands-On CPR Training
EtCO₂ monitoring is a vital tool during CPR, providing real-time, objective insight into the effectiveness of chest compressions, ventilation, and overall circulation. By reflecting the cardiac output generated by compressions, confirming proper airway placement, guiding ventilation, and serving as an early indicator of return of spontaneous circulation, EtCO₂ allows rescuers to make immediate, informed adjustments that can improve patient outcomes. Recognizing that chest compressions are the main determinant of EtCO₂, while also considering secondary influences such as ventilation, pulmonary conditions, medications, and equipment factors, ensures accurate interpretation and maximizes the quality and effectiveness of resuscitation efforts.
While understanding the science behind EtCO₂ is crucial, translating that knowledge into confident, effective action requires hands-on practice. CPR VAM training center offers AHA-certified CPR, BLS, ACLS, and PALS courses designed to equip you with practical skills for high-pressure emergencies. Learn to perform effective chest compressions, manage airways, and monitor EtCO₂ in real time. Take the next step to become a skilled responder and make a difference when every second becomes critical for clinical interventions.